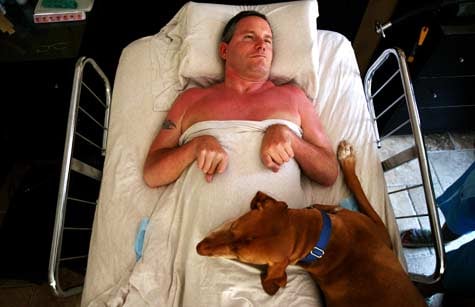
Nurse Owen Jay Murphy Jr. twisted the jaw of one patient until he screamed.
He picked up another one – an elderly, frail man – by the shoulders, slammed him against a mattress and barked, "I said, 'Stay in bed.' "
He ignored the alarms on vital-sign monitors in the emergency room, shouted at co-workers and once hurled a thirsty patient's water jug against the wall, yelling, "How do you like your water now?" according to state records.
Murphy's fellow nurses at Kaiser Permanente Riverside Medical Center finally pleaded with their bosses for help. "They were afraid of him," a hospital spokesman said.
Under pressure, Murphy resigned in May 2005. Within days, Kaiser alerted California’s Board of Registered Nursing: This nurse is dangerous.
But the board didn't stop Murphy from working elsewhere, nor did it take steps over the next two years to warn potential employers of the complaints against him. In the meantime, Murphy was accused of assaulting patients at two nearby hospitals, leading to convictions for battery and inflicting pain, board and court records show.
Even Murphy, who has since taken classes to curb his anger, was surprised the board didn't step in earlier.
 "The nursing board is there to protect the public from me," he said in an interview.
"The nursing board is there to protect the public from me," he said in an interview.
The board charged with overseeing California's 350,000 registered nurses often takes years to act on complaints of egregious misconduct, leaving nurses accused of wrongdoing free to practice without restrictions, our joint investigation investigation with The Times found.
It's a high-stakes gamble that no one will be hurt as nurses with histories of drug abuse, negligence, violence and incompetence continue to provide care across the state. While the inquiries drag on, many nurses maintain spotless records. New employers and patients have no way of knowing the risks.
Reporters examined the case of every nurse who faced disciplinary action from 2002 to 2008 – more than 2,000 cases in all – as well as hundreds of pages of court, personnel and regulatory reports. They interviewed scores of nurses, patients, families, hospital officials, regulators and experts.
Among the findings:
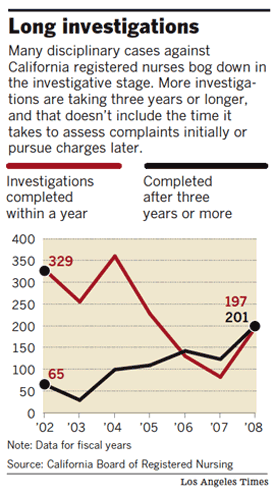
* The board took more than three years, on average, to investigate and discipline errant nurses, according to its own statistics. In at least six other large states, the process typically takes a year or less.
"It's really discouraging that when you do report people . . . they don't take action," said Joan Jessop, a retired chief nursing officer in Los Angeles who filed multiple complaints with the board during her 43-year career. "What is so frightening to me is that these people will go on and do it to somebody else."
* The board failed to act against nurses whose misconduct already had been thoroughly documented and sanctioned by others. Reporters identified more than 120 nurses who were suspended or fired by employers, disciplined by another California licensing board or restricted from practice by other states – yet have blemish-free records with the nursing board.
* The board gave probation to hundreds of nurses – ordering monitoring and work restrictions – then failed to crack down as many landed in trouble again and again. One nurse given probation in 2005 missed 38 drug screens, tested positive for alcohol five times and was fired from a job before the board revoked his probation three years later.
* The board failed to use its authority to immediately stop potentially dangerous nurses from practicing. It obtained emergency suspensions of nurses' licenses just 29 times from 2002 to 2007. In contrast, Florida's nursing regulators, who oversee 40% fewer nurses, take such action more than 70 times each year.
In interviews last week, the board's leaders and other state officials defended its record. "We take what we do – protecting the public – very, very seriously," said Executive Officer Ruth Ann Terry.
Terry, at the helm for nearly 16 years and on staff for 25, acknowledged that the pace of the disciplinary process has "always been unacceptable" and said the system was being streamlined. But she blamed other parts of the state bureaucracy for delays and was vague about what changes would be made.
Later, the state Department of Consumer Affairs, which oversees the board, sent reporters a three-page list of "process improvements." Many were mundane or incremental adjustments – such as revising disciplinary guidelines or planning expert witness training. Others seemed more directly aimed at reducing delays: adding staff, meeting with investigators about stalled cases and using computer systems to better track complaints.
Patricia Harris, acting chief deputy director of the department, stood behind the board. "I think they do a good job," she said.
It's impossible to measure the number of nurses whose conduct endangers patients, but it is presumed to be a small fraction. The board disciplines several hundred a year.
Even a small number of troubled nurses can have wide impact, however. Registered nurses are required to perform or oversee complex treatment, and each can see dozens of patients a week.
Patients generally don't have a choice in which nurse they get. Most trust that, at minimum, the government wouldn't allow a nurse with known problems at their bedside.
In California, the board's vigilance is especially important. The state has among the fewest registered nurses per capita of any state, with an estimated 654 working nurses for every 100,000 residents, compared with 836 nationwide.
Putting even greater strain on the nursing supply is a unique state law that limits how many patients each hospital nurse can treat at one time.
With demand outstripping supply, nurses have readily jumped from one hospital to another, and employers have relied heavily on the board to screen out poor performers.
Despite its critical mission, the board faces little outside scrutiny or pressure to change its ways. Public board meetings, held five times a year, are filled with praise for staffers' efforts. During five meetings attended by reporters since November 2007, Terry never focused on the delays in discipline.
 And board members – including both nurses and public appointees – never publicly challenged staffers or urged quicker action even though they review every disciplinary action. (Board President Susanne Phillips said such questions are often raised with staff privately.)
And board members – including both nurses and public appointees – never publicly challenged staffers or urged quicker action even though they review every disciplinary action. (Board President Susanne Phillips said such questions are often raised with staff privately.)
While the board tarries, nurses like Owen Jay Murphy Jr. keep working.
In 2006, more than a year after Kaiser warned the board about him, Murphy was employed at Riverside Community Hospital. There, according to a criminal investigator's affidavit, he forcibly grabbed the face of a patient whose arms were tied down.
"I was helpless," said Christy Ledebur, now 50. "Why would they have someone like that working in an emergency room?"
Ten days later, Murphy punched and elbowed another restrained patient in the face, the investigator's statement said.
"I don't even recall the first two hits," said Murphy, 41, adding that his stress and anger at the time clouded his memory. "They said I hit 'em three times."
Riverside Community fired him in July 2006 and immediately alerted the nursing board, a hospital official said. He later pleaded no contest to misdemeanor charges in both incidents.
A month later, a patient at Arrowhead Regional Medical Center in Colton complained that Murphy had put her in a headlock and shoved her against the wall, leaving clumps of hair on the bed and floor, according to hospital officials and board records.
The board took its first public action in June 2007, filing a formal accusation detailing the administrative charges against Murphy.
The former Army medic said in an interview that he had been provoked in some cases by aggressive or mentally impaired patients. But he said he was a good nurse and confident that court-ordered anger management classes had taught him self-control.
Still awaiting his first board hearing, he works in the emergency room of Parkview Community Hospital in Riverside with an unrestricted license.
Racking up accusations
The Times and ProPublica found more than 60 nurses disciplined since 2002 who – like Murphy – were accused of committing serious misconduct or mistakes in at least three health facilities before the board took action.
 At least five employers reported Los Angeles nurse Carolyn Fay Thomas to the board for allegedly making medication errors and falsifying charts to hide her drug thefts.
At least five employers reported Los Angeles nurse Carolyn Fay Thomas to the board for allegedly making medication errors and falsifying charts to hide her drug thefts.
And John Michael Jones racked up complaints from at least three hospitals for stealing and using drugs during work. Yet the board waited five years to revoke his license, even after he allegedly dozed off while performing CPR on a dying patient in 2002.
"I was high some of the times that I was working. Yes, I was," Jones, who denies falling asleep during CPR, said in an interview.
Several hospital administrators expressed shock when reporters told them that nurses they had turned in for dangerous failings went on to work at other facilities. No one tracks these nurses, who typically aren't required to tell the board where – or even if – they are working.
"There's got to be a better system than now to protect our patients and their safety," said Deborah Hankins, chief nursing officer at Bakersfield's San Joaquin Community Hospital, one of the hospitals that complained about Jones.
As it stands, complaints often take a circuitous route through several clogged bureaucracies: from the nursing board for initial assessment to the Department of Consumer Affairs for investigation, to the California attorney general's office for case filing and the state Office of Administrative Hearings for trial. Then the case goes back to the board for a final decision.
Other California health licensing boards are also hampered by delays – but the registered nursing board stands out because of the sheer volume of licensees it regulates.
The biggest bottleneck occurs at the investigation stage, as Consumer Affairs staffers struggle to handle complaints against nurses as well as those against cosmetologists, acupuncturists and others. The nursing board must share a pool of fewer than 40 field investigators with up to 25 other licensing boards and bureaus. Some investigators handle up to 100 cases at a time.
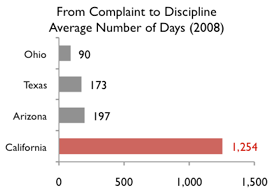
All told, cases closed by the nursing board in fiscal 2008 took an average of 1,254 days. That pace surprised officials at other states' boards.
"I don't think it's ever to anybody's advantage to have a case open for three years," said Valerie Smith, associate director of Arizona's board, which typically takes 6 1/2 months from complaint to resolution.
Nursing boards nationwide vary widely in how they investigate and discipline nurses. But many do it faster.
Officials from Arizona, Texas and Ohio say they handle almost everything within their own agencies, exercising tight control and questioning cases that take too long.
"Where there's the greatest risk, we want to take the fastest action," said Betsy Houchen, head of Ohio's board, which requires 95% of the most serious complaints to be investigated within five working days.
Boards with the fairest and quickest outcomes hire their own investigators, usually nurses themselves, as well as their own attorneys, according to a 2004 trade group report.
Terry could ask the state Legislature for broader authority or permission to hire her own investigators, but she said she has no plans to. Rather, she said, she intends to adhere to the "process that the state of California has set up in terms of protecting the public."
 She said her staff had recently begun working with Consumer Affairs investigators to prioritize and expedite the handling of complaints.
She said her staff had recently begun working with Consumer Affairs investigators to prioritize and expedite the handling of complaints.
It's not a new goal. In a 2002 report to the Legislature, the board said that "there has been a steady and unacceptable increase" in length of disciplinary cases and called for "strategies to expedite cases."
Current and former state attorneys say funding has been an issue – at times they've been asked to suspend work on nursing board cases to save money. But Phillips said the board, which is funded by licensing fees paid by nurses, has enough money. It hasn't raised its fees in 18 years.
There is no legal pressure for the board to act faster. Unlike with disciplinary cases against doctors, there's no statute of limitations on nurses. The delays make the pursuit of cases more difficult: Witnesses die. Records are purged. And former co-workers cannot be found.
Even nurses targeted by the board are frustrated by the slow pace. Kimberly Ann Garza received three years' probation in 2008 – 6½ years after her bosses at a Central Valley hospital complained that she had failed to account for her patients' drugs. At one point, the investigator went on medical leave and Garza's file sat for 11 months before a colleague took it over.
"If I'm such a danger and I'm such a liability, why were they not on top of this?" said Garza, who denied she stole drugs.
A girl questions why
Caitlin Greenwell grinned slyly as she sat before a special computer at her family's ranch home in Lafayette, about 10 miles east of Oakland. Her eyes darted around a keyboard on her screen, as a sensor tracked her gaze and allowed her to spell out words.
"Let's test my mom," she typed, then looked up with a devilish smile. "We will test my mom on math."
Julia Greenwell laughed. "In so many ways, she's typical," she said.
 But the 9-year-old has begun questioning why she is trapped in a wheelchair, unable to control her limbs or speak, said her father, Steven. Caitlin, he said, is "very aware that things didn't go right and some were due to people not doing their jobs."
But the 9-year-old has begun questioning why she is trapped in a wheelchair, unable to control her limbs or speak, said her father, Steven. Caitlin, he said, is "very aware that things didn't go right and some were due to people not doing their jobs."
Like many aggrieved patients and their families, the Greenwells say they feel doubly victimized, first by nurses and then by the board itself. Steven Greenwell said he won't rest until the board disciplines Candyce Warren, the nurse he holds primarily responsible for Caitlin's injuries at birth.
In October 1999, Warren and the trainee she was overseeing missed crucial signs during Julia Greenwell's labor that the baby's condition was deteriorating, according to allegations in a 2000 lawsuit by the Greenwells against John Muir Medical Center in Walnut Creek.
Caitlin was deprived of oxygen and as a result has cerebral palsy, according to the suit, settled in 2003. A doctor paid a separate settlement.
Attorneys for the Greenwells said that Warren was responsible for the trainee, who had little experience reading fetal monitoring strips, and that both nurses tried to cover up their mistakes by altering the medical record.
Steven Greenwell lodged a complaint with the nursing board in June 2003 – waiting, as his attorney advised, until after the civil case was resolved. The board filed an accusation a year or so later. Then the case disappeared into the state's bureaucracy.
There was no word on the matter until 2008, when the board amended the charges against Warren to fault her handling of a different baby's distress back in 2002. That child was stillborn.
Still there was no resolution for the Greenwells and no explanation for the delays. "I kept calling the nursing board and getting nothing," Steven Greenwell said.
Greenwell said he also spent hours on the phone imploring a deputy attorney general to see the case through – only to learn recently that she had left her job.
Warren, who still works at John Muir, feels wronged by the board as well. She disputes the allegations and wants to clear her name but wouldn't discuss specifics while the case is pending. At least five hearings have been set, then put off, she said.
"What they are doing is torturing us," she said. "It's not right."
Multiple alleged lapses
In 2005, Los Angeles County officials fired Abbie Dickerson, a nurse at the publicly owned Olive View-UCLA Medical Center in Sylmar.
She had connected a patient's feeding tube so it leaked into a surgical wound, according to her Sept. 7 termination letter.
It wasn't Dickerson's first alleged lapse. She'd been written up four times for medication errors, according to the letter, which is on file with the county Civil Service Commission.
"Your unsatisfactory job performance and medical errors are no longer tolerable," the letter said. Dickerson's appeal to the commission was thrown out because she failed to show up for a hearing. She declined to comment.
California nursing regulators either didn't know about the allegations or didn't do anything about them – they wouldn't say. Anyone looking Dickerson up on the board's website would find a clean record. She is free to work anywhere in the state.
Hers is one of the 120 cases in which the board hasn't acted despite sanctions imposed by other agencies or employers that were based on clear evidence. Reporters easily found the cases through public records, and nothing prevents the board from getting the same information and acting on it.
Cases like these "should be dealt with immediately," said Agoura Hills nurse Tricia West, an authority on healthcare quality who has been an expert witness both for the board and for nurses accused of wrongdoing.
Even when a registered nurse loses a license with another of California's professional boards, the nursing board does not always act promptly.
In more than a dozen cases, individuals were able to care for patients as registered nurses after they had been severely sanctioned – or even had their license revoked – by the Board of Vocational Nursing and Psychiatric Technicians.
Both boards use the same pool of investigators and fall under the Department of Consumer Affairs. But the department has no central database that can be searched for all the licenses belonging to an individual.
Lynn Teehee lost her LVN license in 2006 following allegations that she had improperly inserted a feeding tube into a patient, then ignored his cries of pain as his abdomen was flooded. The man died two days later of septic shock, records show. Her license was revoked after she failed to respond to the allegations.
The registered nursing board filed its charges two years after the LVN board acted – and later put Teehee on probation.
Percy Randall Wade surrendered his vocational nursing license in 2003 after being accused of failing to account for missing narcotics. Then, while working under his registered nursing license, he billed San Quentin State Prison $161,000 for work he didn't do. He was convicted of felony grand theft in 2006.
A year and a half later, the registered nursing board filed an accusation against him, citing both incidents. He was given four years' probation in March.
The problem extends beyond the vocational nursing board. Dorothy Wilson (also known as Dorothy Bauer) is licensed as both a registered nurse anesthetist and a podiatrist. In 1999, the California Board of Podiatric Medicine put her on five years' probation for repeated acts of negligence.
The following year, as a nurse handling anesthesia during a breast enlargement operation, Wilson did not notice that the patient had stopped breathing, according to filings in a subsequent malpractice suit against Wilson and the surgeon.
 Mary Lopez, then 32, was deprived of oxygen, went into a coma and suffered brain damage, according to the pleadings. Lopez's attorney filed a complaint with the nursing board in April 2002, alleging that Wilson had over-sedated Lopez, then altered records to cover up the error.
Mary Lopez, then 32, was deprived of oxygen, went into a coma and suffered brain damage, according to the pleadings. Lopez's attorney filed a complaint with the nursing board in April 2002, alleging that Wilson had over-sedated Lopez, then altered records to cover up the error.
A judge found Wilson at fault and ordered her in August 2002 to pay Lopez $779,000, although the case was settled for a lower, undisclosed amount on appeal, said Wilson's attorney, Michael Khouri.
The nursing board did not file an accusation against Wilson until December 2007. Wilson's lawyer said in court papers that any injury to Lopez resulted from wrongdoing by the surgeon, not his client. (The surgeon was dropped from the case.)
As for Lopez, she had to relearn her ABCs, her numbers, even how to walk. A clerical worker, she requires notes to remind her each day how to do her job and when to pick up her children.
"I'm not 100% who I was," she said. "She took that away from me."
Data not demanded
The nursing board says it can't act on cases it doesn't know about. But it's not set up to find out what it needs to know, The Times and ProPublica found.
Most states require hospitals to report nurses who have been fired or suspended for harming a patient or other serious misconduct. So, for that matter, does California's vocational nursing board.
Not the registered nursing board.
Heidi Goodman, the board's assistant executive officer, told The Times in 2007 that the board could be overwhelmed if such reports were mandated. "We have to work within existing resources," she said. "You get the flood. What are you going to do about it?"
The board also largely shuts itself off from information about nurses licensed in California who get in trouble elsewhere.
 It is not part of a national compact of 23 state nursing boards that share information about nurses who are under investigation or have been disciplined. And unlike 35 states, California does not put the names of all its registered nurses into an industry database. So if a California-licensed nurse gets in trouble in another state, that state may not know to notify California.
It is not part of a national compact of 23 state nursing boards that share information about nurses who are under investigation or have been disciplined. And unlike 35 states, California does not put the names of all its registered nurses into an industry database. So if a California-licensed nurse gets in trouble in another state, that state may not know to notify California.
Terry said last week that the board would consider requiring California hospitals to report errant nurses – a proposal that has come up before but never gained traction. She also said the board wants to arrange a one-time computer sweep of other states' actions to determine which of them involve California nurses.
Until recently, the state did not even ask nurses renewing their licenses whether they had been disciplined elsewhere or convicted of crimes. It began doing so only after The Times and ProPublica highlighted the loopholes last fall.
This spotty oversight has left some nurses suspended or barred from practice in other states free to care for patients in California.
One of those nurses, Sandra Corrine Taylor, had her license revoked by Oklahoma and Texas. A third state, Idaho, took away her license as a lesser-skilled nurse.
Among her alleged offenses: verbal and physical abuse of nursing home patients, medication errors and lying about her academic credentials, according to records from the other state boards. Taylor could not be reached.
Perhaps the most telling sign of dysfunction is when other states act against nurses for crimes and misdeeds committed in California before California's own board does. Often it appeared they simply had better information and acted on it more quickly.
David Miranda was fired by a Pasadena hospital in 2003 for testing positive for drugs on the job, then convicted in Los Angeles in 2005 of illegal gun possession. Citing those incidents, Arizona's nursing board denied him a license in 2006.
Based in part on Arizona's action, California's board gave Miranda probation in November 2007. Just last month the board moved to pull his license after he failed two drug tests.
Given a second chance
More than half the nurses who respond to allegations from the board are handed a second chance. Each year, California places at least 110 nurses on probation, warning that if they get in trouble again, their licenses may be yanked.
In reality, such action seldom happens quickly, if at all, according to a review of hundreds of nurse disciplinary records.
Just five board monitors oversee about 470 nurses on probation. Often nurses must undergo physical and mental exams, take drug tests, submit to workplace monitoring and attend rehabilitation or support groups.
But when they don't meet some – or any – of those requirements, years often pass before the board tries to revoke their probation.
At times the punishment for violating probation is more probation.
One nurse was put on three years' probation in 1996 for stealing drugs from a Sacramento hospital. After she ignored numerous requirements, her probation was extended three more years in 1999, according to board documents. Finally in 2003, after she relapsed, skipped drug tests, was convicted of possessing codeine and Valium without a prescription, got a job without permission and missed support group meetings, her license was revoked.
But last year, the board found the nurse had "demonstrated sufficient rehabilitation" and gave her license back – with probation.
Carolyn Claeys, now 61, was put on probation in July 2005. The home healthcare nurse had showed up for work drunk and had stolen drugs from a former patient's house, according to her board disciplinary record.
At the time, Claeys also had three criminal convictions: two for drunk driving and one for petty theft.
Nursing board documents describe what happened next:
Less than four months into her nursing board probation, Claeys was convicted of a DUI. Four months after that, she was fired from a nursing home for stealing drugs. She tested positive for drugs three times between November 2005 and March 2006 and missed 12 required drug tests.
Any of these violations would have been grounds for the board to revoke her probation. But the board took no action – at least none that could be found in public records.
 In July 2006, Claeys was found passed out, high on drugs, in the Santa Cruz apartment of Dorothy "Jeanie" Rising, who had died of cancer the previous day. Claeys, one of her caregivers, admitted to authorities that she'd stolen Rising's painkillers and injected them.
In July 2006, Claeys was found passed out, high on drugs, in the Santa Cruz apartment of Dorothy "Jeanie" Rising, who had died of cancer the previous day. Claeys, one of her caregivers, admitted to authorities that she'd stolen Rising's painkillers and injected them.
Five months later, the board filed a petition to revoke Claeys' probation. She didn't contest the charges, and her license was later revoked.
In an interview, Claeys acknowledged that she was "an impaired nurse." But she said she'd waited until Rising was dead to steal the drugs.
"It wasn't that horrific," she said, "as opposed to if I had been sitting right there when I was there with her: 'Here, one for you, one for me.' "
Terry said that adding probation staff should help. "You won't find that happening anymore," she said of such cases.
As for other improvements, she cautioned that they would take time.
"It's not going to happen overnight," Terry said.
See our database of sanctioned nurses
Doug Smith, The Times’ director of database reporting, contributed to this report.